
Releasing Scars. Restoring Freedom.
Overcoming the Limits of Burn Contractures.
When burn scars heal tightly over a joint, they can lock the neck, arms, or fingers in place. M.Ch. Plastic Surgeon Dr. Pawan Shahane specializes in advanced surgical release techniques to instantly unlock joints, alleviate pain, and restore your natural range of motion.
Schedule a ConsultationUnderstanding the Mechanics of a Contracture.
Skin is incredibly elastic; it stretches effortlessly every time you bend your elbow or turn your neck. However, when the skin suffers a deep burn (2nd or 3rd degree), the body replaces it with rigid, fibrous scar tissue. As this scar matures, it naturally pulls together and shrinks. If this shrinking happens across a joint, it acts like a permanent, invisible cast, severely restricting movement.
This is known as a burn contracture. It cannot be permanently fixed with stretching alone. Dr. Pawan Shahane approaches contracture release as an intricate architectural puzzle. By surgically altering the direction of the scar tissue and introducing new, healthy skin, we can release the tension and allow the joint to move freely once again.
Advanced Release Techniques
Tailoring the reconstruction to the severity of the scar.
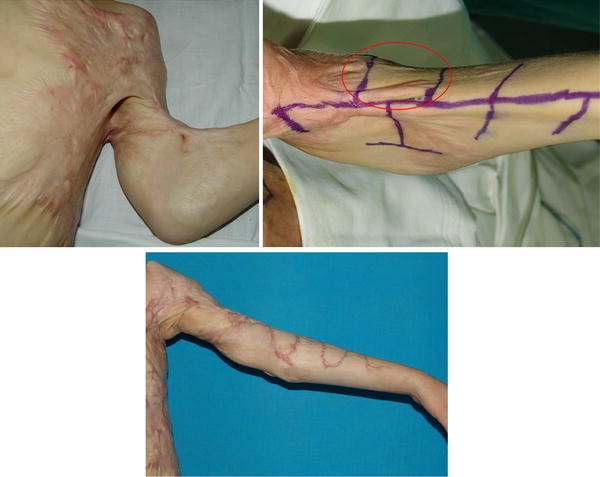
Z-Plasty & Tissue Rearrangement
For linear scar bands that restrict a joint, Dr. Pawan uses a classic plastic surgery technique called Z-Plasty. By cutting the scar in a precise "Z" shape and transposing the tissue flaps, the tight scar is instantly lengthened and redirected, removing the tension.
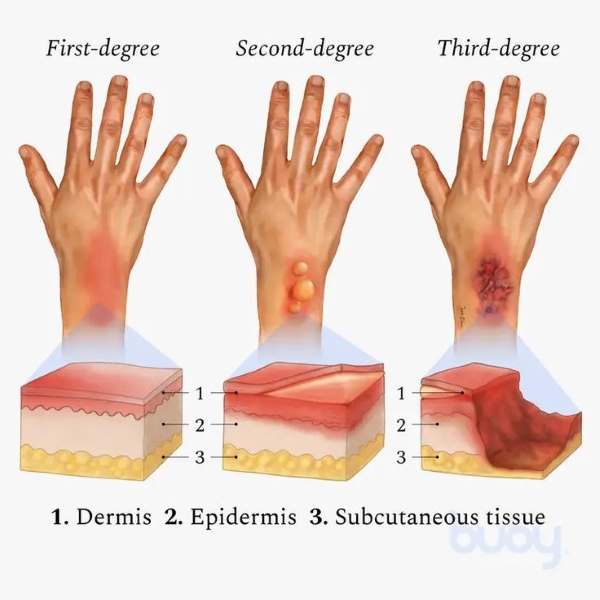
Excision & Skin Grafting
When a large area of thick scar tissue covers a joint (like the front of the neck), Z-plasty alone is not enough. The scar must be completely cut away, allowing the joint to release. The resulting gap is then covered with a healthy skin graft taken from the thigh.
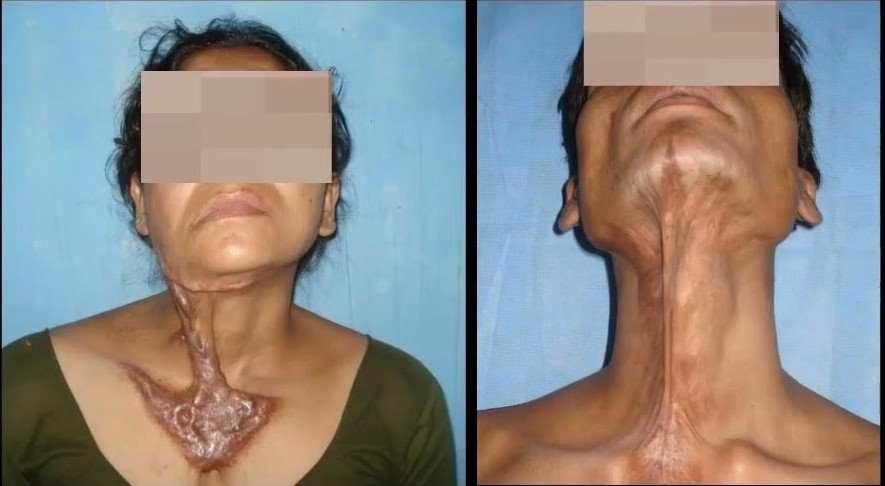
Regional Flap Surgery
For very deep contractures where releasing the scar exposes underlying tendons, nerves, or bone, a simple skin graft will not survive. Dr. Pawan will rotate a thicker "flap" of nearby healthy skin and fat to provide durable, flexible coverage over the vital structures.
The "Re-Contracture" Prevention Protocol
The biggest risk of contracture surgery is that the new surgical wounds heal tightly, causing the contracture to return. We utilize aggressive post-operative management to prevent this.
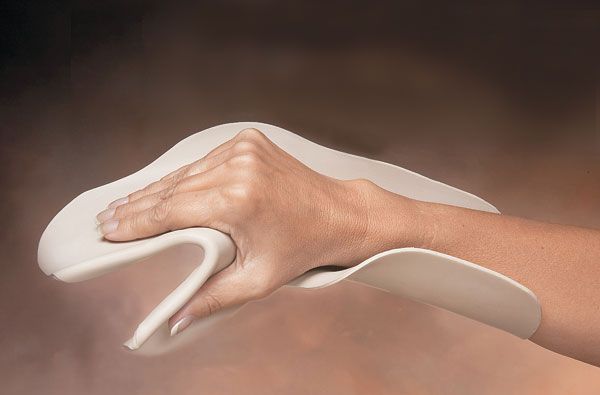
Intraoperative Splinting
While you are still under anesthesia and the joint is fully released, we apply a custom plaster or thermoplastic splint holding the joint in its new, fully stretched position. This ensures the graft heals precisely at the correct length.
Targeted Physiotherapy
Surgery provides the potential for movement, but physiotherapy makes it permanent. We coordinate with specialized hand and burn therapists to ensure you begin guided movement exercises as soon as the grafts are secure.
Pressure & Silicone Therapy
To prevent the margins of the new grafts from thickening into new scars, we prescribe the immediate use of custom compression garments and medical-grade silicone sheets, maintaining a flat, soft result.